FDA Advisers Overwhelmingly Oppose Approval of MDMA As a Psychotherapeutic Catalyst
The panel's recommendation, based on several concerns about two clinical trials, is a serious setback for a promising PTSD treatment.
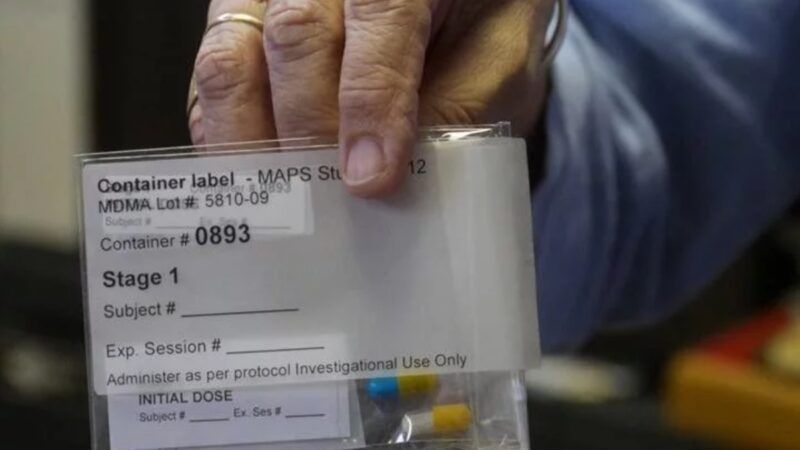
Efforts to make MDMA legally available as a psychotherapeutic catalyst hit a daunting roadblock on Tuesday when an expert panel overwhelmingly voted to recommend that the Food and Drug Administration (FDA) reject a new drug application that Lykos Therapeutics submitted in February. Members of the panel expressed several concerns about two Phase 3 studies of MDMA's safety and effectiveness in treating post-traumatic stress disorder (PTSD), including unblinding of subjects, potential underreporting of adverse events, and allegedly inadequate assessment of MDMA's abuse potential.
"We are disappointed in today's vote given the urgent unmet need in PTSD and appreciate that the committee faced a challenging and atypical assignment, which was to evaluate a therapeutic approach that combines drug therapy (MDMA) and psychological intervention," said Amy Emerson, CEO of Lykos Therapeutics, a company created by the Multidisciplinary Association for Psychedelic Studies (MAPS). "We remain committed to working with the FDA to address outstanding questions so that we may find a path forward to ensure the responsible and careful introduction of MDMA-assisted therapy into the healthcare system, if approved."
Nine of the 11 advisory committee members concluded that MDMA's effectiveness has not been demonstrated, while 10 agreed that its benefits do not outweigh its risks. "It seems like there are so many problems with the data," said panelist Melissa Decker Barone, a Department of Veterans Affairs psychologist. "Each one alone might be OK, but when you pile them on top of each other…there's just a lot of questions I would have about how effective the treatment is."
The two clinical trials compared subjects who received MDMA in conjunction with psychotherapy to subjects who underwent the same sort of therapy but received placebos. On their face, the results of those studies are impressive.
The first study, published by Nature Medicine in 2021, involved 90 subjects with "severe PTSD," as measured by the Clinician-Administered PTSD Scale for DSM-5 (CAPS-5). That questionnaire is designed to assess problems such as "intrusive distressing memories," hypervigilance, an exaggerated startle response, sleeplessness, difficulty in concentrating, avoidance of cues reminiscent of a traumatic event, and "feelings of detachment or estrangement from others." The second study, reported in the same journal two years later, involved 104 subjects with "moderate to severe PTSD." Both studies found that subjects who received MDMA saw larger reductions in their CAPS-5 scores than the control group.
The differences were substantial. On average in the 2021 study, CAPS-5 scores, which range from 0 to 80, fell by more than 24 points in the MDMA group, compared to about 14 points in the placebo group. At the end of the study, two-thirds of the MDMA group "no longer met the diagnostic criteria for PTSD," compared to a third of the control group. In the 2023 study, the average score decreases were about 24 points and about 15 points, respectively. More than 70 percent of the MDMA group no longer qualified for a PTSD diagnosis, compared to 48 percent of the control group.
One reason the FDA's advisers discounted these results is the likelihood that subjects, who were randomly assigned to the two groups and theoretically did not know whether they were taking MDMA, surmised which group they were in based on the presence or absence of the drug's expected effects. The researchers described the placebo as "inactive," meaning it did not even have the stimulating effect of MDMA, so it would not have been hard for subjects to figure out what they got. "Although we do have two positive studies," said FDA clinical reviewer David Millis, "the results are in the context of dramatic functional unblinding."
A May 2024 report from the Institute for Clinical and Economic Review (ICER) raised the same issue. "Because of the effects of MDMA, the trials were, essentially, unblinded," it said, "with nearly all patients who received MDMA correctly identifying that they were in the MDMA arm of the trials. This would always raise concerns about bias, but these concerns are particularly heightened as we heard from multiple experts about the very strong prior beliefs of those involved in the trials (as investigators, therapists, and patients) about the benefits" of MDMA-assisted psychotherapy.
A functional lack of blinding is undeniably a problem for any study that tries to rigorously measure a drug's benefits, especially when the measured outcome is psychological. Critics of SSRI antidepressants such as Prozac, for example, argue that clinical studies exaggerate their benefits because they fail to take into account the possibility of an enhanced placebo effect among subjects who inferred that they had gotten the real thing based on the drug's side effects.
When a drug has recognizable psychoactive effects, as MDMA does, this problem is hard to overcome. One partial solution is to use an active placebo that mimics some physiological effects of the drug. Psilocybin researchers, for example, have given control subjects niacin or a low dose of psilocybin itself. But that approach does not fully prevent unblinding, since the same psychoactive effects that researchers are studying are an obvious clue for subjects in the treatment group.
In the case of MDMA, it is hard to imagine how a truly and fully blind study could be conducted, given the distinctive effects that users have long reported. The psychonautical chemist Alexander Shulgin, who publicized the compound's previously unappreciated qualities, said it "enabled me to see out, and to see my own insides, without reservations." His account stimulated interest in MDMA's psychotherapeutic potential, which predated the "emergency" ban that the Drug Enforcement Administration (DEA) imposed in 1985.
Therapists and clients reported dramatic breakthroughs facilitated by MDMA, which they said made it possible to overcome psychological barriers and confront traumatic memories without overwhelming fear. The recreational use that alarmed the DEA likewise highlighted the drug's distinctive effects, including camaraderie and emotional openness. As far as the FDA is concerned, that anecdotal evidence does not count. But without it, there would have been no interest in systematic research. At the same time, the subjective effects for which MDMA became famous pose an unavoidable challenge for researchers trying to meet the FDA's requirements.
Unblinding was not the only concern expressed by the FDA's advisers. They also worried that the negative effects of MDMA-assisted psychotherapy may have been underreported.
In the 2021 study, the researchers noted that some "treatment-emergent adverse events" were more common in the MDMA group. But they said those effects "were typically transient" and "mild to moderate in severity." They included "muscle tightness, decreased appetite, nausea, hyperhidrosis [excessive sweating] and feeling cold." The authors added that "no increase in adverse events related to suicidality was observed in the MDMA group."
The results of the 2023 study were similar. The authors said psychiatric adverse events, most commonly suicidal ideation, insomnia, and anxiety, "occurred at a similarly high frequency in both groups." ICER, however, said its meta-analysis of the two studies "found very low certainty evidence that there was no increase in suicidal ideation."
According to the 2023 study, no incidents of "MDMA abuse, misuse, physical dependence or diversion" were reported. Millis apparently deemed that suspicious. "We noticed a striking lack of abuse-related adverse events," he said. While that could be due to underreporting, it also could be due to a lack of such events.
"Concerns have been raised by some that therapists encouraged favorable reports by patients and discouraged negative reports by patients," ICER said, "including discouraging reports of substantial harms, potentially biasing the recording of benefits and harms." ICER added that it was "not able to assess the frequency of misreporting of benefits and/or harms and thus the overall balance of net benefit."
To give you a sense of what the FDA might count as a worrisome MDMA effect, NPR reports that "another potential sticking point was the lack of data about how patients experienced the acute effects of the drug, including feelings like 'euphoria' or 'elevated mood.'" Such data, NPR notes, help "inform the FDA's assessments of the drug's abuse potential."
If MDMA helps people overcome severe psychological problems that have plagued them for years, in other words, that counts as a benefit. But if it also makes them feel good, that is problematic and potentially harmful.
More understandably, panel members were alarmed by "sexual misconduct" involving two therapists, a married couple, who participated in the MDMA research. MAPS investigated those complaints, which involved inappropriate physical contact during therapy and a sexual relationship between a therapist and a subject that developed after the study, and confirmed ethical violations. As a result, the therapists "were barred from all MAPS-related activities and from becoming providers of MAPS-affiliated MDMA-assisted therapy if the treatment is approved."
That incident, while obviously troubling, does not fundamentally affect the validity of the MDMA studies. The most serious concern on that score seems to be the lack of effective blinding, which is an intractable problem "because of the effects of MDMA," as ICER noted. It would be paradoxical if the very effects that make MDMA interesting and potentially beneficial became an insurmountable obstacle to FDA approval.
Although the FDA does not have to follow an advisory panel's advice, it typically does. Where that leaves years of effort to win regulatory approval for MDMA-assisted psychotherapy is unclear. I reached out to Rick Doblin, the founder and former executive director of MAPS, for comment on the criticism voiced by the panelists and will update this post if and when I hear back.
Back in 2018, the FDA recognized MDMA as a "breakthrough therapy," meaning it "may demonstrate substantial improvement over existing therapies on one or more clinically significant endpoints." That designation was supposed to facilitate MDMA's approval as a prescription drug. So was the FDA's decision to give the Lykos application "priority review."
The reasons for those decisions remain compelling: MDMA seems to help many people who have unsuccessfully tried other options, often in such a dramatic way that its benefits seem obvious. "PTSD can result in debilitating symptoms that can significantly impact nearly all areas of a person's life," Harvard psychiatrist Jerry Rosenbaum notes in a Lykos press release. "While we have available treatments, unfortunately many people don't respond or stop treatment early….Research has suggested the unique properties of MDMA may act as a catalyst to enhance psychotherapy, the current standard of care, by helping diminish the brain's fear and avoidance responses and extend[ing] the window of tolerance of painful emotions and memories, thereby allowing people to access and process painful memories without being overwhelmed."
Validating those benefits in a way that satisfies the FDA seems to have proven more difficult than MAPS anticipated. Back in 2017, Doblin, who has been defending the psychotherapeutic use of MDMA for decades, was hoping to win FDA approval by 2021. But counting on a habitually overcautious regulatory agency to authorize legal access via medical gatekeepers was always an iffy prospect. And notwithstanding its improbable success until now, that approach implicitly concedes the government's authority to decide who may use which psychoactive substances, when, and why. Unlocking MDMA's full potential might require a radically different understanding of the state's role in policing our brains.

