Will the COVID-19 Vaccines Soon Crush the Pandemic?
The vaccines are great news, but the winter still looks bleak.

As calamitous as the COVID-19 pandemic is, humanity would have been in a much worse situation had it occurred even ten years earlier. The past decade of remarkable biotechnological progress enabled public health officials and researchers to identify the COVID-19 virus, sequence its genome, ramp up diagnostic testing, and then create and begin to deploy numerous vaccines in less than a year.
This week, the United Kingdom approved the Pfizer/BioNTech vaccine. British citizens will begin inoculations next week. The U.S. Food and Drug Administration (FDA) will meet on December 10 to consider an emergency use authorization for that vaccine, and will discuss authorizing the Moderna vaccine a week later. If all goes well, the campaign to vaccinate Americans will begin shortly thereafter. The two companies could supply enough doses to cover around 20 million Americans before the end of the year.
However, even if it was logistically possible to distribute such great quantities of doses, vaccine makers (including Johnson & Johnson and AstraZeneca, in addition to Pfizer/BioNTech and Moderna) do not yet have the capacity to inoculate everyone immediately. So earlier this week, the Centers for Disease Control and Prevention's (CDC) Advisory Committee on Immunization Practices recommended prioritizing vaccination for the 21 million health care workers and the 3 million elderly residents in long-term care facilities. Vaccinations will then be offered to segments of the population at greater risk—essential workers, Americans older than 65 years, and those with comorbidities.
So when is the rollout of the COVID-19 vaccines likely to begin to shift the trajectory of the pandemic? Keeping in mind the problems associated with managing complex logistics and the flaws of epidemiological models, let's take a look at the projections from the Institute for Health Metrics and Evaluation (IHME).
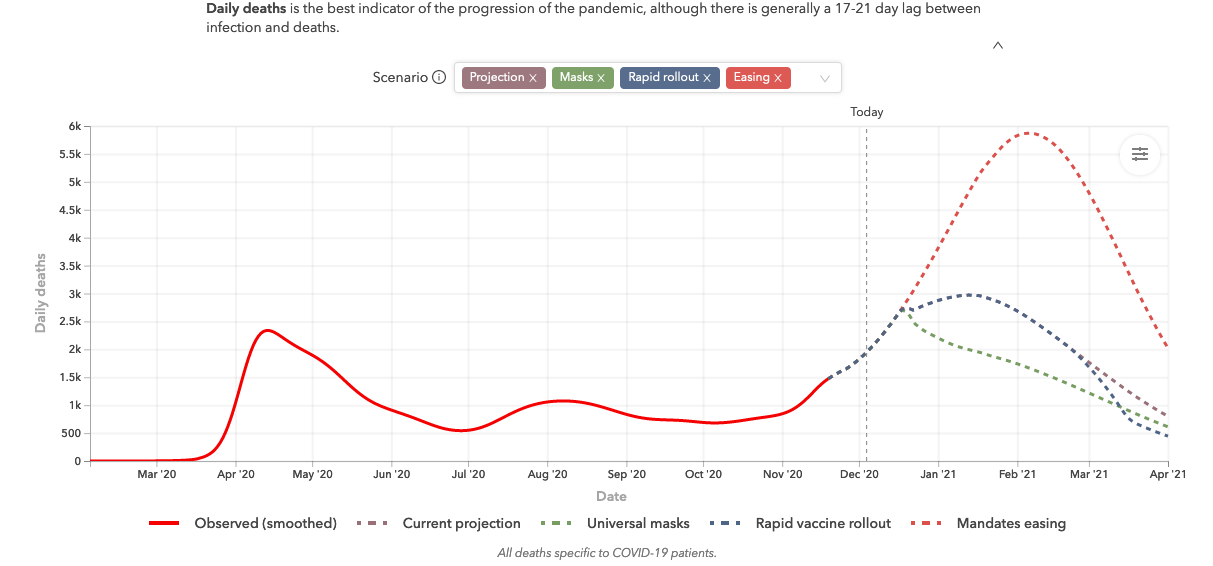
Even assuming a rapid rollout of the vaccines, the IHME projects that they will not really begin changing the current trajectory of daily COVID-19 deaths until around February. In the meantime, what does work is wearing facial coverings to prevent the spread of the virus.
"The vaccine has not come in time to do much about the winter wave," said Christopher Murray, director of the IHME, in The Washington Post. "Vaccination is coming too late even if we do a really great job of scale-up. It's coming too late to do much by March 1, or really by April 1." Only at that point, he added, will the widespread distribution of vaccines begin to crush the virus.
Here's to hoping that the IHME projections are too pessimistic about how much help vaccines will render throughout the coming winter. For now, social distancing, mask-wearing, and proper hygiene remain key to blunting the pandemic's course for the next few months.



Show Comments (189)