Vaccine-Related Heart Inflammation Risks for Young People Much Lower Than COVID-19 Heart Inflammation Risks
Young males infected with COVID-19 are six times more likely to develop myocarditis than those who have been vaccinated.

Currently, the mRNA COVID-19 vaccine produced by Pfizer/BionNTech is approved for people age 12 and older, whereas the Moderna vaccine is approved for those over age 18. If the current clinical trials in younger children prove successful, both vaccines will seek Food and Drug Administration (FDA) approval for inoculating children between ages 5 and 11 years later this year.
As vaccines are further rolled out to younger cohorts, recent reports that in rare instances adolescents have experienced inflammation of their hearts (myocarditis) shortly after being inoculated with mRNA COVID-19 vaccines have understandably alarmed some parents. Although researchers are still trying to work out how the vaccines might cause this ailment, researchers have reported a correlation between vaccination and the onset of this side effect. The good news is that in the vast majority of cases the heart inflammation is safely resolved after a few days. So far, no one in the U.S. diagnosed with myocarditis after vaccination has died.
On balance, most research finds that the risks of this side effect in adolescents and young adults are outweighed by the risks from COVID-19 infection. For example, an August 25, 2021, New England Journal of Medicine (NEJM) study by Israeli researchers used nationwide data from that country's largest health organization to compare the incidence of myocarditis among thousands of people inoculated with the Pfizer/BioNTech vaccine, unvaccinated people, and infected COVID-19 patients. The researchers report that, while still quite rare, vaccinated people experienced myocarditis at a rate just over three times higher than the unvaccinated. But more crucially, people infected with COVID-19 had 18 times higher risk than people who were not infected with COVID-19. In other words, the currently uninfected face the choice, with respect to heart inflammation, between the lower risks of vaccination versus the considerably higher risks of infection. More importantly, the health downsides of COVID-19 infections are not limited to just a higher risk of heart inflammation compared to those who are vaccinated.
As an accompanying NEJM editorial noted:
What is even more compelling about these data is the substantial protective effect of vaccines with respect to adverse events such as acute kidney injury, intracranial hemorrhage, and anemia, probably because infection was prevented. Furthermore, the persons with SARS-CoV-2 infection appeared to be at substantially higher risk for arrhythmia, myocardial infarction, deep-vein thrombosis, pulmonary embolism, pericarditis, intracerebral hemorrhage, and thrombocytopenia than those who received the BNT162b2 [Pfizer/BioNTech] vaccine.
A July 27, 2021, preprint analysis of the health records of 48 large U.S. healthcare organizations compared the heart inflammation risks of people under age 20 between those who had suffered a COVID-19 infection versus those who had been vaccinated. As with other studies, the researchers found that young males are, for unknown reasons, at greater risk of the malady than are young females. Overall, the researchers report that "young males infected with the virus are up 6 times more likely to develop myocarditis as those who have received the vaccine."
A September 3, 2021, article assessed the data for more than 36 million patients supplied by over 900 hospitals focusing on myocarditis and COVID-19 cases in the Centers for Disease Control and Prevention's (CDC) Morbidity and Mortality Weekly Report. The researchers stratified the data by age and sex. They note that myocarditis is rare with patients with and without COVID-19. The researchers report, "During March 2020–January 2021, patients with COVID-19 had nearly 16 times the risk for myocarditis compared with patients who did not have COVID-19, and risk varied by sex and age."
In contrast to these relatively reassuring data and analyses, another preprint article posted on September 8, 2021, seeks to parse adolescent heart inflammation data derived from the Vaccine Adverse Event Reporting System(VAERS). Those researchers compare post-vaccination heart inflammation risks with the risks of being hospitalized with COVID-19 infections in the next 120 days. They report that that the rate of post-vaccination heart inflammation for boys ages 12-15 (males being more susceptible) without medical comorbidities is 3.7 to 6.1 times higher than their 120-day COVID-19 hospitalization risk as of August 21, 2021. For boys ages 16 to 17 without medical comorbidities, the risk is currently 2.1 to 3.5 times higher than their 120-day COVID-19 hospitalization risk.
However, the VAERS site warns users that because of significant reporting biases, inconsistent data quality and completeness, and the absence of an unvaccinated comparison group, its data cannot be used to calculate how often adverse events occur and cannot assess if a vaccine caused an adverse event.
Over at the Science-Based Medicine blog, Wayne State University oncologist David Gorski argues that the authors of this preprint have in any case misunderstood and badly mishandled the VAERS' self-reported data about COVID-19 vaccinations. Among other things, he points out that the researchers are not comparing apples to apples when they contrast vaccine-related cases of heart inflammation with COVID-19 hospitalizations instead of cases of vaccine-related inflammation with COVID-19 inflammation cases. In addition, he asks why the authors chose not to compare vaccine-related hospitalizations of children with COVID-related hospitalizations of children?
As it happens, a July 20, 2021 study in Circulation made just that comparison.
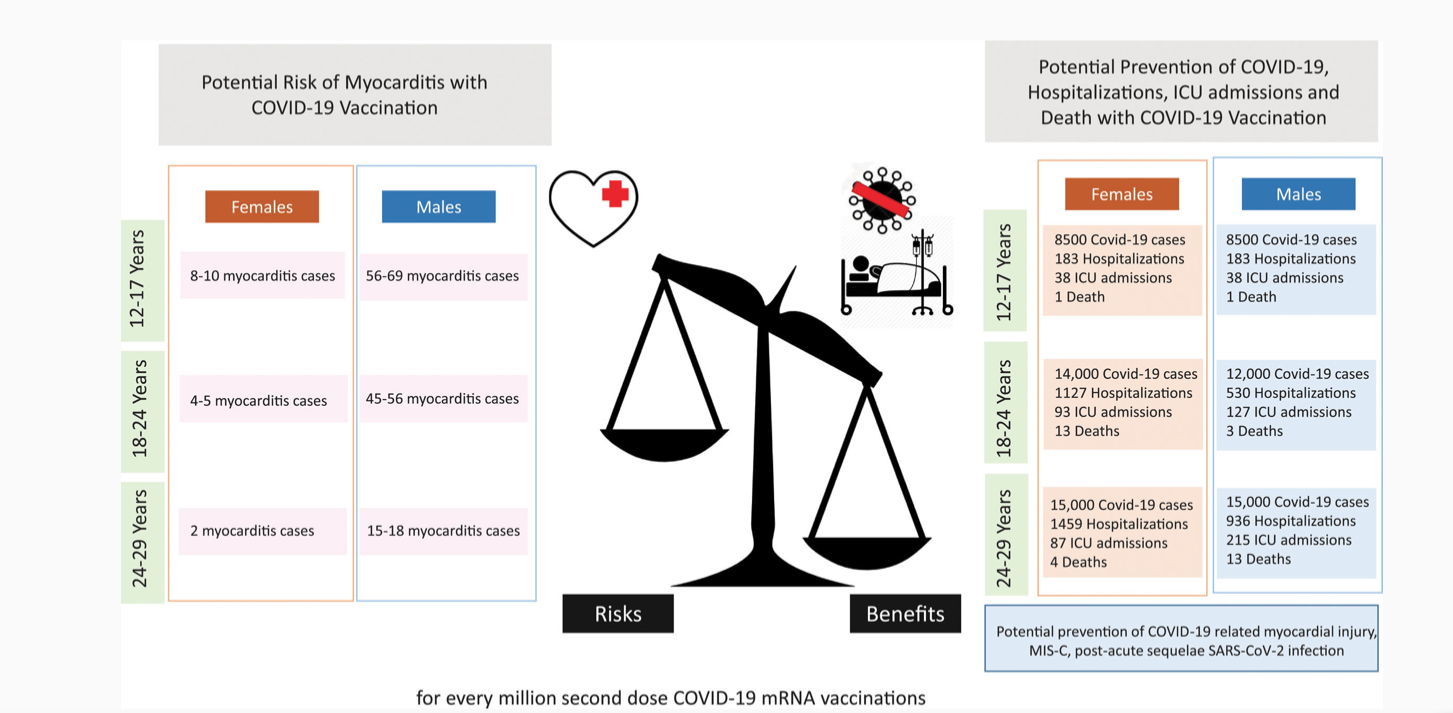
A slightly different comparison of the myocarditis risks for younger people versus the risks of remaining unvaccinated was put together for the August 30, 2021, meeting of the Advisory Committee on Immunization Practices by National Center for Immunization and Respiratory Diseases cardiologist Hannah Rosenblum.
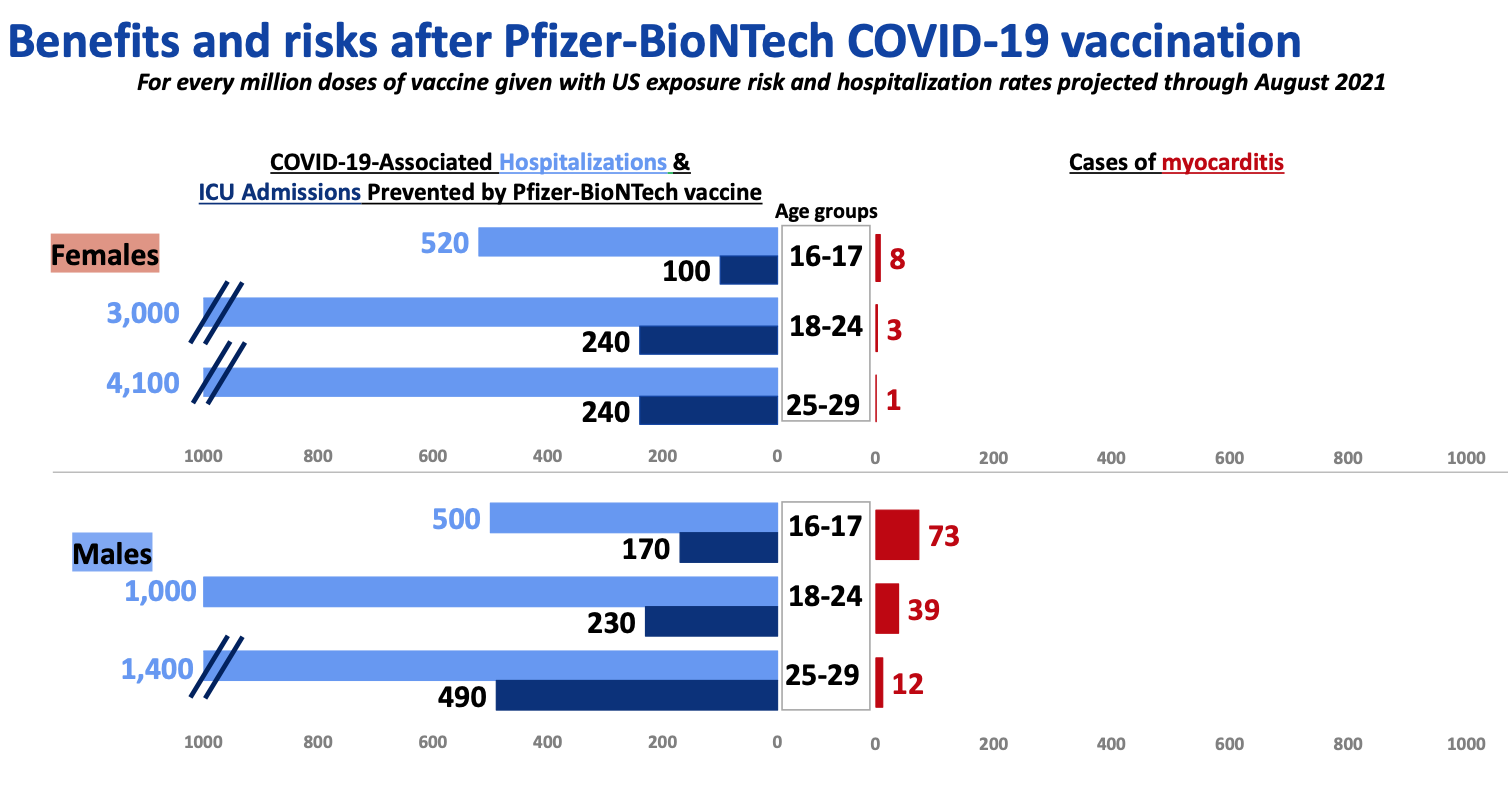
After reviewing the evidence for vaccine-related myocarditis in young people, an August 27, 2021, editorial in the European Journal of Internal Medicine concluded:
At this point in time, very rare cases of myocarditis in younger adult men can occur following COVID-19 vaccination, but they are clinically mild and with benign evolution. To date, the benefit-risk assessment for COVID-19 vaccination shows a favourable balance in light of the potential of short- and long-term major cardiovascular and non-cardiovascular complications associated with this disease and the long life-expectancy of this population.
Therefore, COVID-19 vaccination is strongly recommended to prevent major complications and death.
Given current data and analyses, that seems about right.



Show Comments (113)