U.S. Cancer Incidence and Death Rates Fall to a 25-Year Low
Good news: The cancer death rate which stood in 1991 at 215 per 100,000 people has dropped in 2016 to 156 per 100,000 people.
"The overall cancer death rate dropped continuously from 1991 to 2016 by a total of 27 percent, translating into approximately 2,629,200 fewer cancer deaths than would have been expected if death rates had remained at their peak," notes the American Cancer Society (ACS) in its latest annual update of cancer mortality and incidence statistics. In 1991, the cancer death rate stood at 215 per 100,000 people and has fallen in 2016 to 156 per 100,000 people. The report also notes that the cancer death rate between 2007 and 2016 for both women and men declined annually by 1.4 and 1.8 percent, respectively.
In addition, the ACS reports that the cancer incidence rate between 2006 and 2015 for women has been stable while dropping by approximately 2 percent per year for men. In other words, the modern world is not producing an epidemic of cancer as predicted by so many activists.
Most of the decline in both incidence and mortality is due to reductions in smoking tobacco (which increases the risk of a number of cancers, particularly lung cancer) and advances in the early detection and treatment of cancer. According to the report, LiveScience notes, lung cancer death rates have dropped by 48 percent among men from 1990 to 2016; and 23 percent among women from 2002 to 2016. Breast cancer death rates dropped 40 percent among women from 1989 to 2016; prostate cancer death rates dropped by 51 percent among men from 1993 to 2016; and colorectal cancer death rates dropped by 53 percent among both men and women from 1970 to 2016. The reduction in death rates for breast, prostate, and colorectal cancer reflect the use of screening tests that result in earlier detection and, in the case of colorectal cancer, the removal of precancerous polyps during colonoscopy.
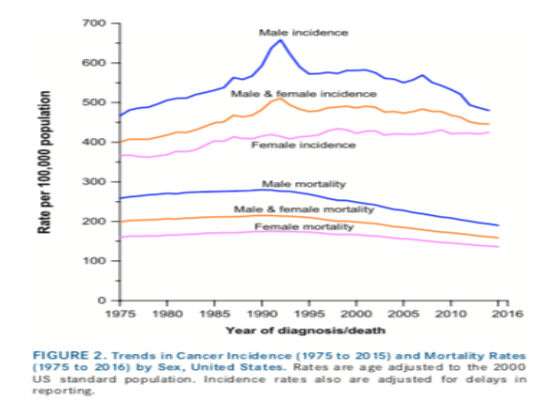
The news is not all good, however. Incidence rates for melanoma, liver, and thyroid cancers in men and women since 1975 have trended slightly upwards.
The report does also note that compared with the most affluent counties, mortality rates in the poorest counties were two-fold higher for cervical cancer and 40 percent higher for male lung and liver cancers during 2012-2016.
Overall, the chances that an American man will be diagnosed with cancer before age 49 is 1 in 30, rising after age 70 to 1 in 3. For American women the chances of being diagnosed with cancer before age 49 is 1 in 18, rising after age 70 to 1 in 4. Still, the lifetime probability of being diagnosed with invasive cancer is slightly higher for men (39.3 percent) than for women (37.7 percent).
The report notes that the disparity between men and women is possibily associated with sex differences in immune function and response. Adult height is also positively associated with cancer incidence and mortality in both men and women, and has been estimated to account for one-third of the sex disparity.*
*Disclosure: This correlation is annoying given that I am six feet and five inches tall.

