No, Simply Touching Fentanyl Can't Kill You
An anesthesiologist explains fentanyl 101.
For all the ink American media outlets have spilled covering the increase in fentanyl-related overdose deaths, few of the stories I've read explain how fentanyl works or why it's so deadly.
As a result, journalists have created the impression that fentanyl is a magically awful drug. In that sense, it has a lot in common with PCP, methamphetamine, and crack cocaine. "Using [crack] even once," ABC's Peter Jennings declared in a 1989 episode of World News Tonight, "can make a person crave cocaine for as long as they live." If there's an equally believable-but-untrue claim about fentanyl, it's that simply touching the stuff can kill you.
I thought it might be useful for other reporters, and people who are simply concerned and/or curious about fentanyl, to figure out which oft-reported claims are true, partially true, or flat out wrong. So I got in touch with the Stanford anesthesiologist Steven Shafer, an expert in the pharmacology of pain medicine. I've edited our exchange for length and clarity.
Q: How do street-level doses of fentanyl—which seem to range from less than a milligram to a few milligrams—compare to surgical doses?
A: A milligram of fentanyl is a huge dose, one that would be fatal. For surgery we typically use doses of 0.1 milligram (100 micrograms). In terms of street drugs, the high potency has a very practical implication: The stuff is difficult to measure. There would be no obvious difference to a user given a packet of fentanyl-laced heroin if it had a very small amount of fentanyl, or a guaranteed fatal dose of fentanyl. The user would need to trust whomever weighed out the fentanyl used to lace the heroin.
Q: What makes illicitly used fentanyl deadlier than other opioids?
A: Fentanyl effect peaks at 5 minutes after an intravenous injection. The fast onset is more likely to be fatal than a slow onset, because the body doesn't have time to build up carbon dioxide. With a slow onset opioid (e.g., morphine), breathing slows gradually as the drug starts to act, and carbon dioxide rises. As carbon dioxide rises, it drives ventilation, offsetting (somewhat) the effects of the morphine on breathing. With the rapid onset of fentanyl, there is little time for carbon dioxide to raise before there is full effect of the fentanyl on depressing breathing. That will result in more lethality for the same maximal opioid drug effect.
Q: What do we mean when we say fentanyl is "x times more potent" than other opioids?
A: Potency is usually given for opioids by the amount (by weight) of drug required to achieve a particular drug effect. For example, one could use the "Minimal Effective Analgesic Dose," basically the lowest dose of a drug that produces some amount of pain relief. Potency can also be discussed in terms of tissue concentration, what is the plasma concentration of drug that produces a particular effect.
Because of differences in pharmacokinetics (drug uptake, distribution, and metabolism), differences in dose and differences in concentration may vary several-fold. The rate of blood brain equilibration also makes a difference. Fentanyl effect peaks at five minutes after an intravenous injection, and it's washed out by 90 minutes. Because it has slow blood-brain equilibration, morphine effect is quite modest at five minutes, but peaks at 90 minutes. Thus, it's tricky to talk about one drug being X-fold more potent than the next, because it depends on exactly when you measure drug effect. At five minutes? At 90 minutes? You will get very different answers for relative potency depending on exactly when you make your measurements.
If one says that fentanyl is 50 times stronger than drug X, you can't tell from the statement if that means that it takes 1/50th of the dose, or if it requires 1/50th of the concentration. Thus, the key concept is that fentanyl is gobs more potent than drug X, so you need a very small fraction of fentanyl compared to the other drug to get a big effect. It's not more scientific than that, because so many details affect how the potency is calculated and compared.
Q: Is it possible to develop a tolerance to fentanyl? Are users at higher risk of overdose due to lack of tolerance if they inadvertently take fentanyl mixed into a non-opioid formulation?
A: Tolerance develops to all opioids. Fentanyl is no better, or worse, than others. However, tolerance is shared: Tolerance to heroin will make the addict also tolerant to fentanyl. Tolerance also occurs with benzodiazepines. If an addict who is tolerant to valium mixes it with a "normal" amount of fentanyl, and then takes a whopping dose of valium, they may overdose from the fentanyl.
Q: EMTs have reported needing larger doses of naloxone to reverse fentanyl overdoses. Does that sound correct?
A: It depends on the dose. Fentanyl is displaced from the mu opioid receptor just like morphine, oxycodone, or any other opioid. Naloxone will work just fine. However, because fentanyl is so potent, the person mixing it into heroin might make a 10-fold dose error. In that case, it will take 10 times the amount of naloxone. So there's nothing magic about fentanyl, other than that it is so potent that it's hard to get the dose right when you are using crude scales to mix it together.
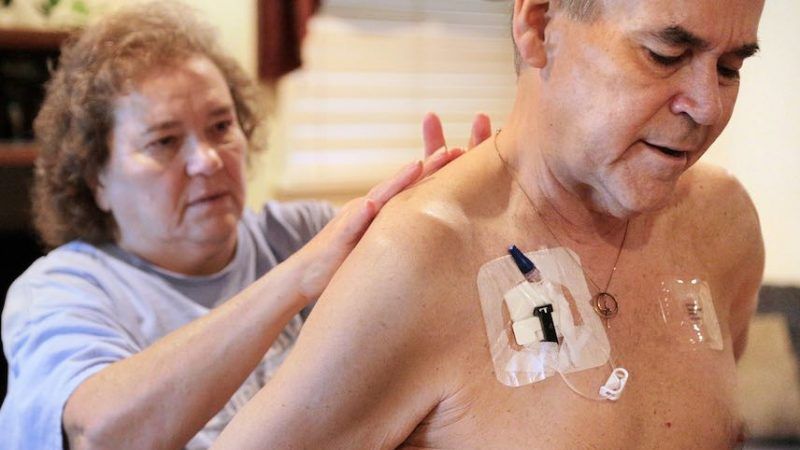
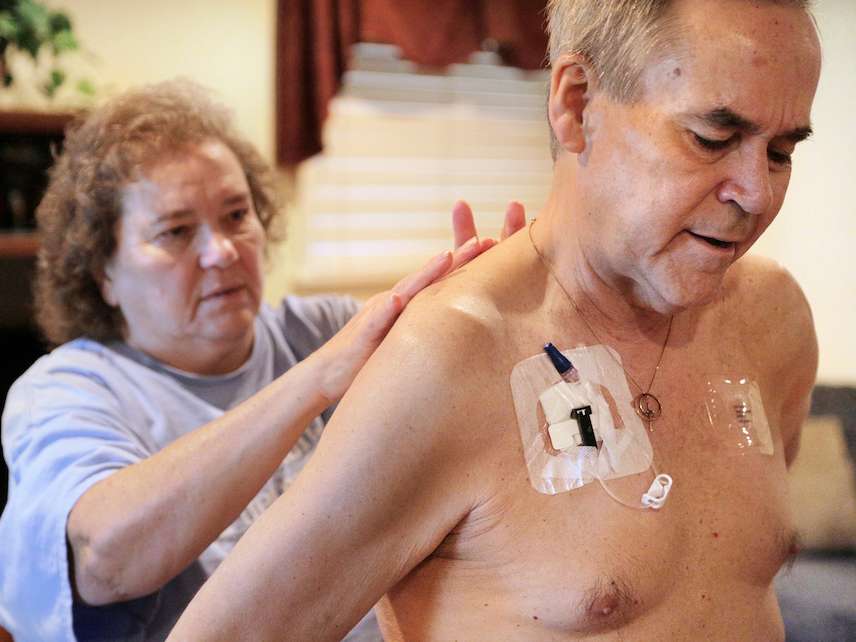
Q: Is fentanyl dangerous to touch, as several law enforcement agencies have reported?
A: No, fentanyl is not dangerous to touch. Transdermal fentanyl patches deliver fentanyl across the skin, but they require special absorption enhancers because the skin is an excellent barrier to fentanyl (and all other opioids). However, it is readily absorbed through mucus membranes, so snorted, rubbed in the mouth, or swallowed are all effective ways of administering fentanyl.
Q: Does fentanyl produce a better high than other opioids?
A: It isn't fundamentally different from other opioids, like heroin, morphine, or oxycodone. In terms of drug effect, an opioid is an opioid is an opioid. They all bind at the mu opioid receptor, and they all have the same fundamental properties. So fentanyl isn't going to give addicts a better high. Addicts like the "rush" of the fast onset, so they might prefer the fentanyl rush to the onset of a slower opioid like morphine. However, the net opioid effect will be the same.
Q: In terms of what various public health agencies are doing globally to reduce overdose rates, what kind of strategies do you think are worth trying in the U.S.?
A: This is a very complex question! There are several parts to the answer. First, we need to develop better strategies of managing pain. A lot of addiction starts with opioids given for pain management. This is because there is almost no pain that cannot be managed effectively for a short time by opioids. In other words, opioids are very effective short-term analgesics. There seems to be nothing else that can replace them. We need to find ways to limit opioid use for chronic pain, except at the end of life, because they cause addiction and lead to dependence. The other problem is that we need better ways to treat psychological pain. Psychological pain is handled by the same brain pathways that handle physical pain. That's why we use the same word, "pain," for both. Opioids are effective for psychological pain as well, but they are a terrible choice.
Q: Are there any harm reduction strategies that might reduce fentanyl overdose rates specifically? I know some facilities in Canada offer free reagent testing, but I've also seen it argued that reagent testing is not an effective way to identify fentanyl in a mixture.
A: That would work, as long as it is sufficiently sensitive. One could readily make over the counter fentanyl detection kits so that addicts could identify if their concoction has been laced with fentanyl. That would likely be a good idea.

